Did you know that each year, millions of people battle kidney disease? The National Kidney Foundation estimates that roughly 10% of the global population is affected by CKD in some capacity. In forwarding the dialogue around kidney health education, we collaborated with ANC’s Dr. Alec Otteman to break down different types of kidney disease and tips to stay on top of your kidney health. If you enjoy this blog, we hope you share what you’ve learned with friends and loved ones to further promote kidney disease awareness in 2025. Happy reading!
Causes of Kidney Disease and Stages
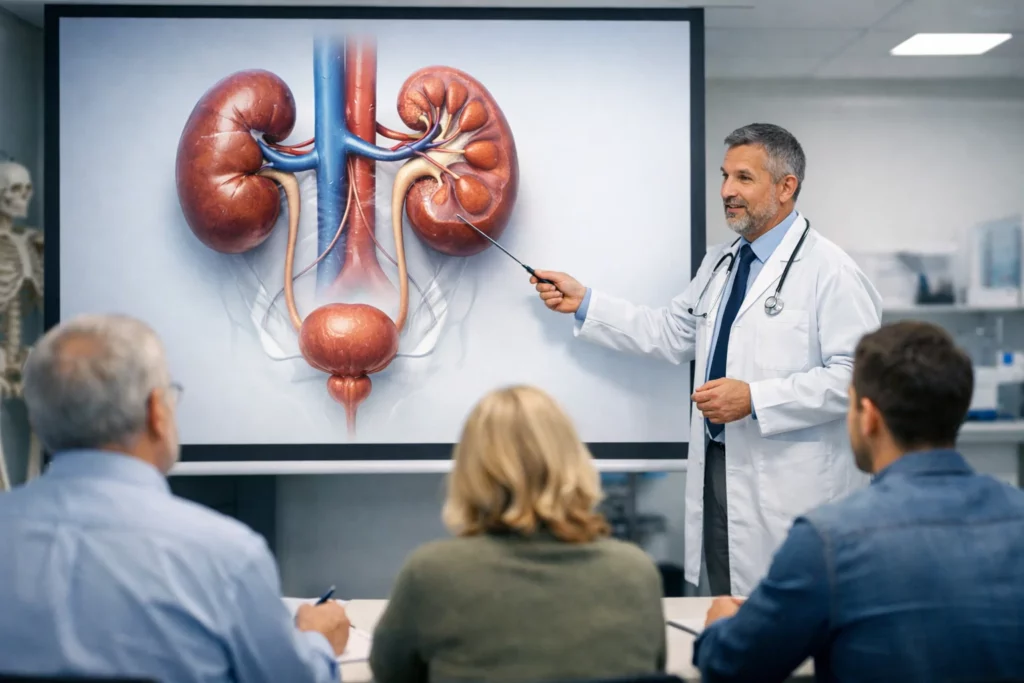
Kidney disease can stem from a variety of causes. The most common types doctors tend to see are diabetic kidney disease and hypertensive kidney disease. Diabetic kidney disease typically develops in long-term diabetes patients who have lived with their condition for 10-15 years. Hypertensive kidney disease on the other hand is often linked to consistently high blood pressure and heart disease. There are many other much less common types of kidney disease ranging from genetic to autoimmune and one of a nephrologist’s main jobs is to help patients diagnose which type they have.
The progression of kidney disease can also vary between different people. Dr. Otteman states that what they typically see in patients is a mild case that slowly worsens over time, especially in tandem with poorly maintained co-morbidities. Kidney disease progresses through five key stages with stages 1 and 2 being early and most often associated with certain rare types of kidney disease. Stage 3 kidney disease is very broad and encompasses anything from mild asymptomatic disease to much more concerning and rapidly progressive disease. Patients typically become aware of their condition through routine monitoring done by their primary care provider and may begin connecting with a nephrologist to help navigate through their diagnosis. Stage 4 kidney disease is when patients begin showing more signs and symptoms of kidney disease and conversations about transplant and dialysis occur. Finally, stage 5 is when patients typically need a transplant or dialysis.
The progression of kidney disease can seem scary, but we are fortunate that in recent years we’ve seen significant new and exciting therapies being developed that are starting to fundamentally change how kidney disease is being managed. We are hopeful about the impact this research may bring!
Acute Kidney Injury vs. Chronic Kidney Disease
Acute Kidney Injury (AKI) refers to a sudden, temporary decrease in kidney function. AKI often takes place when the body is facing infection, dehydration, or sometimes adverse reactions to medication. In many cases, AKI is reversible with proper medical care. AKI is a very common complication in patients hospitalized for other medical issues and patients can frequently encounter nephrologists in these settings. In contrast, Chronic Kidney Disease (CKD) is often a gradual, long-term decline in kidney function that tends to stem from some of the comorbidities we discussed earlier. Once the kidneys lose function in CKD, it is unlikely that they will fully recover. Careful management and monitoring can be crucial in ensuring something minor like AKI doesn’t snowball into a larger issue like CKD.
How to Stay On Top of Your Kidney Health
Some of the best ways to take care of your kidney health are by making intentional health choices and self-monitoring for symptoms. If you notice symptoms like fluid retention, poorly controlled blood pressure, or changes in urine (very foamy urine or blood in the urine), these could be early signs of kidney issues. As kidney disease progresses, symptoms like appetite changes, increased itching, and rapid swelling may appear.
The most essential way to prevent later-stage kidney disease is attending all your necessary check-ups with primary care providers and catching it early. Primary care providers are the first line of defense against kidney disease and if you have risk factors like diabetes and high blood pressure it is crucial to have routine monitoring through your primary care clinic to evaluate things like creatinine levels, blood pressure, and urine tests. If any issues arise, your primary care doctor can recommend corrective actions right off the bat or refer you to a nephrologist for more specialized care.
Broader Impact of Kidney Disease
Early detection is a crucial step in the fight against kidney disease which is why organizations like the National Kidney Foundation provide localized screening opportunities to raise awareness and provide resources to find kidney care if they need it. Kidney disease can also be a risk factor for many other types of health problems including cardiac disease and other blood vessel disease. Kidney disease can also have a significant impact on aspects of your health like anemia or bone density.
At ANC, our team is dedicated to spreading credible provider-sourced information to help our community navigate the challenge of CKD. If you are interested in helping with this message, we invite you to look into volunteering opportunities in partnership with your local organizations to drive greater impact.